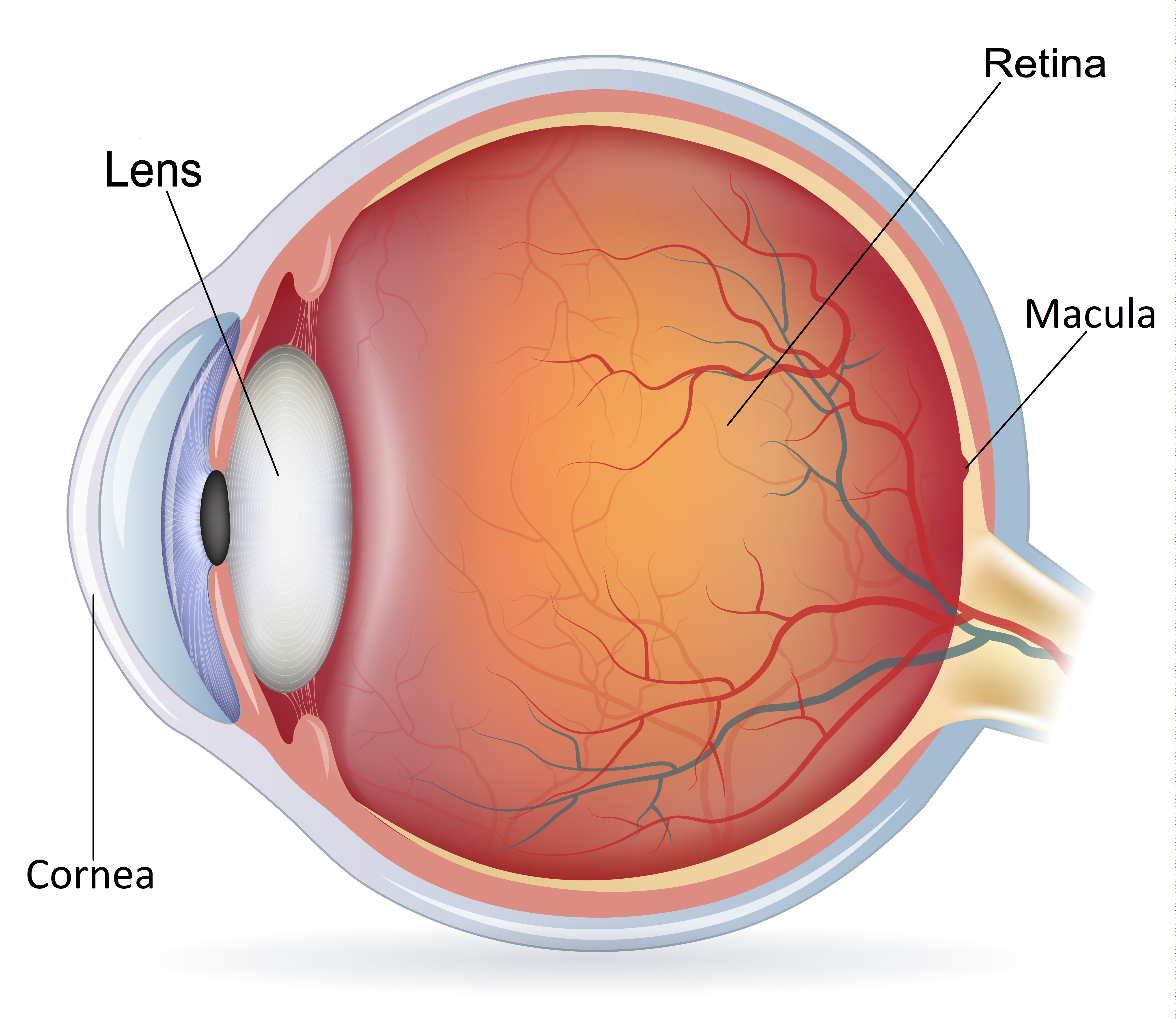
The eye is like a camera with a lens in the front and the retina is the light-sensitive film at the back of the eye. An epiretinal membrane is a condition where a thin layer of scar tissue forms on the surface of the retina. When this membrane grows over an area called the macula (an important area responsible for our sharp central vision) on the retina, it causes wrinkling and crumples up the macula, leading to distorted and/or blurred vision.
In the majority of patients, epiretinal membrane develops due to the normal aging changes inside the eye. In some cases, it can be related to other conditions like diabetes, blockage of retinal blood vessels, inflammation, or previous retinal surgery. The prevalence of epiretinal membrane can vary, but it is estimated to affect approximately 2-5% of the general population. Epiretinal membrane is also called Cellophane maculopathy or Macular pucker.

In many patients, epiretinal membrane is an incidental diagnosis made during a routine eye examination, and it may not affect vision. However, in some patients, the membrane can cause the retina to warp and wrinkle, resulting in distorted and blurred vision. Straight lines may appear wavy, and objects may appear larger or smaller than they actually are. These symptoms may become more noticeable when the affected eye is covered.



Though epiretinal membrane can be diagnosed by clinical examination, it is necessary to do OCT scan of retina, to get intricate details of epiretinal membrane to advice about the surgical outcome. Mr Viswanathan has access to the state-of-the-art retinal scanner to investigate the epiretinal membrane.

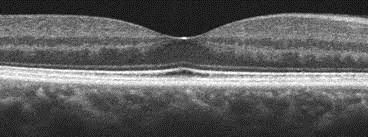

In many patients, epiretinal membrane is an incidental diagnosis made during your routine eye examination and your vision may not be affected initially. These epiretinal membranes tend not to progress and do not typically require treatment if they do not cause significant distortion or blurring of vision that impacts the patient's quality of life. However, if they do get worse and if you have significant distortion and/or blurring of your vision which begins to affect your quality of life then the only way to treat it is to remove the membrane surgically to reduce visual distortion.
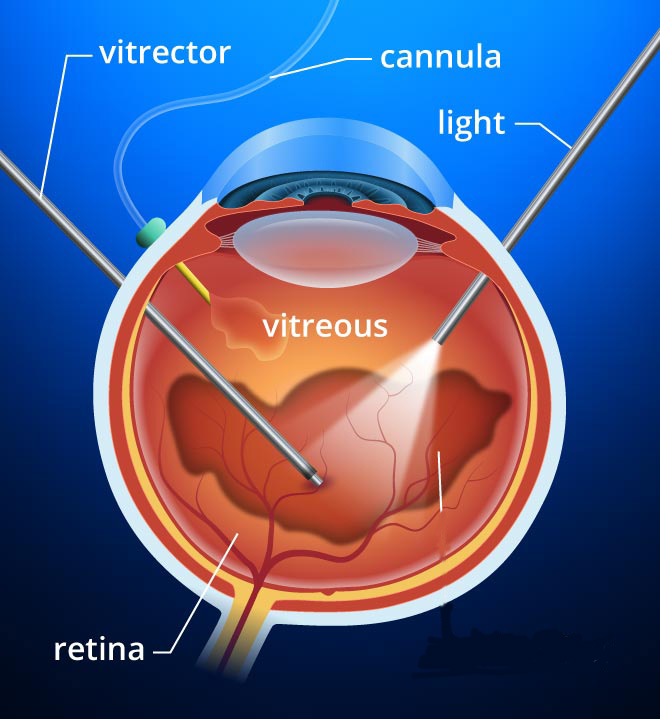
The epiretinal membrane is removed by a procedure called vitrectomy and epiretinal membrane peel. This surgical procedure involves the removal of the vitreous jelly (Vitrectomy) from inside the eye to gain access to the membrane, which is then peeled away from the central part of the retina. The vitrectomy surgery is performed through three small incisions in the eye, which typically do not require suturing.
In some cases, a special gas bubble is left inside the eye, which will dissolve on its own after a few weeks. If gas is used, you may be asked to position your head in a certain ways for most part of the day, typically for 7 days. During this time, it is important to avoid flying or going to high altitudes until the gas bubble disappears. The operation to remove the epiretinal membrane is performed as a day case procedure under local or general anaesthesia, and it usually takes about an hour. If there is also a cataract present along with the epiretinal membrane, both conditions can be addressed in a single combined procedure.
Epiretinal membrane peel surgery is successful in the vast majority of patients, as 80 to 90% of patients undergoing this surgery notice improved vision with a decrease in visual distortion. Much of the visual improvement occurs in the first few weeks, although it can take up to 6 months for the full extent of improvement to be realized.
Understanding epiretinal membrane surgery can be complicated. The information given above will not cover all the concerns you may have about this procedure. Further information can be found at the following websites:
https://www.rnib.org.uk/eye-health/eye-conditions/epiretinal-membrane https://beavrs.org/epiretinal-membraneThe information mentioned here is based on a variety of sources, including latest published research and the Britain & Eire Association of Vitreoretinal Surgeons.
It is impossible to diagnose and treat patients without complete eye examination by an ophthalmologist. I hope the above information will be of help before and after a consultation which this information supplements and does not replace. This information must not be used as a substitute for professional medical care by a qualified doctor or other health care professional.
If you have any concerns about your condition or treatment, please ask your surgeon Mr Viswanathan. We are not responsible or liable, directly or indirectly, for ANY form of damages whatsoever resulting from the use (or misuse) of information contained in this page or found on web pages linked to from this page.
